Shock Wave Therapy for Arthritis in Dogs
A new form of therapy offers pain relief using sound waves
Article by Mary Straus published in the Whole Dog Journal, May 2008
Also see these related articles:
See Also:
Introduction
Last June, I received this note from Debbie Efron, of Manalapan, New Jersey: “Do you know anything about shock wave therapy for dogs with arthritis? I am considering this treatment for Taylor, my almost 13-year-old Labrador Retriever, who has arthritis in her hips, spinal column, and right hock, and has just torn a ligament in her right knee. It was recommended by my vet, Dr. Charles Schenck, who is a past president of the American Holistic Veterinary Medical Association.”
Shock wave therapy? Is that like what they did to the Bride of Frankenstein? I had never heard of such a thing, and I was skeptical, to say the least, thinking it might be some new gimmick. But I was surprised and immensely intrigued by what I found.
Shock waves have nothing to do with electric shocks. They are actually high-energy focused sound waves generated outside the body that can be focused at a specific site within the body. In human medicine, extracorporeal shock wave therapy (ESWT) been used for over 25 years to break up kidney stones and gallstones (lithotripsy) without the need for invasive surgery (“extracorporeal” means “outside the body”). ESWT is also called acoustic compression therapy (ACT).
In 1992, doctors began using shock waves to treat a range of orthopedic conditions, including nonunion of bone fractures; plantar fasciitis (a cause of heel pain); tennis elbow and other forms of tendonitis; rotator cuff injuries; femoral head necrosis; and joint pain. New research is being done on the use of shock wave therapy to speed healing of wounds and burns, and other applications are under investigation.
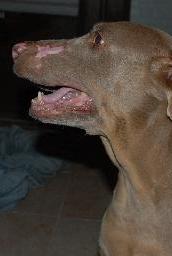
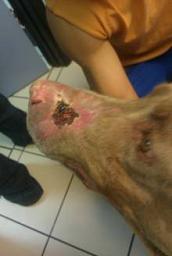
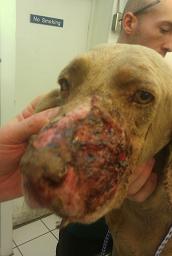 Photo on left is of a dog who was severely mauled by a coyote. The wound became septic and the dog was scheduled to be euthanized, but the vet agreed to try shockwave therapy. Treatment was done with DermaGold using soft-focused waves. The first treatment was done under anesthesia, with two follow-up treatments done without anesthesia. Center photo shows wound 19 days after first treatment. Photo at right shows the wound completely healed approximately 45 days after the first treatment.
Photo on left is of a dog who was severely mauled by a coyote. The wound became septic and the dog was scheduled to be euthanized, but the vet agreed to try shockwave therapy. Treatment was done with DermaGold using soft-focused waves. The first treatment was done under anesthesia, with two follow-up treatments done without anesthesia. Center photo shows wound 19 days after first treatment. Photo at right shows the wound completely healed approximately 45 days after the first treatment.
History of veterinary use
By the late 1990s, veterinarians began exploring the use of ESWT on horses to speed healing of broken bones (including those that failed to heal normally), treat tendon and ligament injuries, and ease the pain of arthritis.
The use of ESWT for horses has been evaluated at a number of veterinary schools, including Iowa State University, the University of Tennessee, Purdue University, the University of Wisconsin, Colorado State University, and the University of California at Davis. It has also been studied extensively in Europe, where it originated. Clinical trials demonstrate that ESWT is effective in treating musculoskeletal disorders that include bone spavin, stress fractures, navicular syndrome, bowed tendon, bucked shin, arthritic joints, and more.
Experimental treatment of dogs using ESWT began in 1999, and several of the schools listed above have been actively involved in this research. Good results have been reported for treatment of various orthopedic conditions in dogs, but the number of controlled clinical studies is still very limited. Conditions likely to benefit from this treatment include:
UpdateIn a podcast on Pet Life Radio's "The Pet Doctor" on April 17, 2011, the host spoke with Dr. Ed Leeds, a board-certified veterinary surgeon in Los Angeles, about his experiences over the last three years with extracorporeal shockwave therapy. He talked about success in treating lumbosacral stenosis (cauda equina syndrome), among other conditions. He would like to try treating Legg-Calve-Perthes disease as well, but feels it must be done before the condition becomes advanced. He also mentioned that dogs should be off NSAIDs and prednisone when the treatment is done, as they feel the inflammatory response can help the healing. Listen to Shocking New Treatment Options for Pets, episode 112, for more information. |
- Osteoarthritis of the shoulder, hip, back, elbow, knee, wrist and ankle
- Hip dysplasia
- Chronic back pain – relief of muscle pain due to spondylosis deformans, chronic intravertebral disk disease, and lumbosacral instability
- Osteochondrosis lesions (OCD)
- Sesamoiditis – inflammation caused by degeneration of small knuckle bones in the foot that can cause persistent lameness, particularly in racing Greyhounds and Rottweilers
- Tendon and ligament injuries
- Tendonitis
- Fractures (non-union or delayed-healing)
- Lick granulomas
- Cruciate ligament injury – can speed healing after surgery, and may also assist dogs with partial tears to improve without the need for surgery
Most studies show significant improvement in a majority of animals treated, but this treatment is still in the experimental stage, and results are not always consistent. As use of ESWT becomes more widespread, it is likely that overall results will improve as more is learned about how this methodology is best applied and procedure protocols are refined.
Small animal practitioners interviewed in 2003 reported that approximately 70 percent of their patients demonstrated a remarkable response to treatment. Another 15 percent exhibited improvement that was not as significant as the first group. Some of these may improve further with a second treatment. About 15 percent show no improvement. Shoulders, backs and hips seemed to respond best to ESWT, while treatment of knee injuries had the least response.
According to SanuWave, makers of the VersaTron shock wave devices for horses and small animals, most cases demonstrate very significant improvement within a week. A second shock wave treatment two to three weeks later often improves the results further.
Taylor’s first treatment
I passed along my findings to Efron, and told her that if Taylor were my dog, I would definitely proceed with the therapy – in fact, I wanted to try it with my dog Piglet, who has severe degenerative joint disease in both elbows, but I was having difficulty finding a practitioner in my area.Dr. Schenck felt that ESWT would benefit Taylor’s hips and hock, and might possibly help her knee as well. He did not recommend it for the spine because he felt it works better where there is more soft tissue. He continued treating the spine with acupuncture instead. Dr. Schenck recommended a total of two sessions, three to four weeks apart, and told Efron to expect gradual improvement over six to eight weeks, with some regression possible in between treatments. Ultimately, he hoped for 80 percent improvement that would last six to seven months.
A few days after the first treatment, Efron sent me this report. “Taylor is greeting me at the door with a toy in her mouth, something she stopped doing weeks ago,” Efron said. “She is eager to go for walks and pulls me around the block, with no limping and her back legs no longer buckle. She is playful again, wanting to wrestle and play ‘steal the sock.’ She is still stiff getting up, though, and cannot make it up the stairs in the house, though she will go up six stairs to go outside, without the need for support as she did before.”
While at the office for Taylor’s first treatment, Efron met a Golden Retriever with severe elbow arthritis, who had difficulty walking by age two. After ESWT treatment at age three, he was able to walk without a limp. He was returning a year and a half later for another treatment.
How does it work?
ESWT devices generate a series of focused high-pressure acoustic pulses (sound waves) that travel from the probe through the skin and soft tissue. When the waves meet tissue interfaces of different densities, such as where soft tissue, tendons, ligaments, cartilage and bone meet, the energy contained in the shock waves is released and interacts with the tissue, producing both mechanical and cellular effects.The shock waves appear to relieve pain and stimulate healing within the injured tissue, although the mechanism for these effects is unclear. Researchers believe that ESWT stimulates the body’s own resources to speed healing, including increasing vascularization (blood supply) to the area being treated, and increasing osteoblastic activity resulting in accelerated bone growth, as well as other factors. The shock waves can also break up calcium deposits that are sometimes associated with tendonitis.
The reason that this treatment relieves arthritis pain is even less clear, but may have to do with depletion of neuropeptides that lead to the sensation of pain and can contribute to the inflammatory response. Shock waves do not appear to slow the progression of osteoarthritis, but rather reduce the pain associated with it.
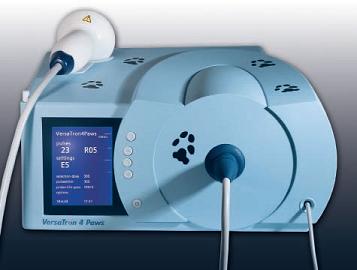
ESWT devices consist of a box that generates the waves, and a wand (probe) that is used to target the waves to specific spots.
How shock wave therapy is performed
A physical exam is required to diagnose musculoskeletal disorder and to rule out neurological disease that cannot be treated with ESWT. It’s important to identify all the painful areas that should be treated, including secondary issues that may have developed due to compensation for an injured or painful joint. X-rays are usually required to help determine treatment, and other standard tests such as blood work and urinalysis may be done to ensure your dog is healthy prior to anesthesia.Discomfort during treatment can range from mild to severe depending on the intensity used, so animals are usually heavily sedated or given short-acting general anesthesia. Low-intensity treatment may be done under light sedation. Pain medication, such as butorphanol, is given before the treatment. The machines that generate the pulses can be quite loud, which may be frightening to the patient, though some devices are quieter than others.
It takes only a few minutes to treat each site. The area to be treated must be shaved and a gel applied to ensure transfer of energy from the probe head to the patient’s tissues, as any air between the probe and the skin will interfere with the mechanism. The veterinarian determines the energy level used and the number of pulses delivered based on the location, type and severity of the disorder.
Protocol varies, but commonly anywhere from one to four treatments are done, two weeks to a month apart. The dog may be a little more sore for a few days following treatment, though sometimes the opposite is true and the treatment produces a short-term anesthetic effect, during which time you must be careful that your dog doesn’t overdo it. Improvement may be seen right away, or it may take a few weeks to see the full effects of the treatment. The process may need to be repeated around once a year.
Update May 2017: The new PiezoWave2 Vet Unit uses Piezoelectric Crystals to produce the high pressure sound waves and it has made ESWT machinery smaller, more affordable, and more accessible for animals to receive treatment without sedation, since it is less painful not as scary or loud to use! It can even be used on small animals now.
TRT's VetGold device is also smaller now and almost pain-free, no anesthesia required.
Taylor’s second treatment
Taylor experienced some regression two weeks after her first treatment, getting up more slowly and becoming more reluctant to go up steps. This may be partly due to the ruptured knee ligament, as she avoided pressure on that leg when she could. A second treatment was done three weeks after the first, and her improvement gradually resumed.Six weeks following the second treatment, Efron reported, “I am quite pleased with the results – Taylor is almost her old self! Walks are getting longer, up to a mile with no limping or buckling, but still quite slow. She is swimming again twice a week, which she loves. She runs down a ramp, retrieves a toy we throw in, comes out of the water and wants us to chase her around the outside of the pool to get the toy again. She is on no medications at all, and she is happy.”
Taylor still has limitations. “She will never run again,” says Efron. “She won’t go up the steps in the house, but she climbs the steps to go outside much better now. She still gets sore at times, such as after a long car ride.”
Four months after treatment, Efron sent me an update. “I think Taylor is still improving somewhat. She does all of our old walks no problem, just a little slower. She even wants to chase her ball occasionally. We built a ramp off our deck, so she doesn't have to use the steps to go out, but she is doing better going up the flight inside our house at bedtime.”
Safety Issues
ESWT is generally considered safe, though high-intensity or prolonged treatment (beyond 1,000 pulses) might be capable of damaging tissue or bone. The energy intensity matters more than the number of pulses. It is possible that the analgesic (pain-relieving) effect can lead to overuse, which would make injury more likely, so it’s important to moderately restrict activity as needed for a few days following treatment.Care must be taken during treatment to avoid the brain, heart, lungs and intestines, as well as neurovascular structures (major nerves and blood vessels). ESWT is not recommended for dogs with clotting disorders due to the potential for bruising. Dogs that are immune-compromised may not respond as well to therapy, which is thought to rely on the body’s own immune system for healing.
With proper use, side effects are insignificant, limited to some bruising of the skin where the pulses are applied if bubbles are present or good contact with the probe cannot be achieved. Treatment requires an in depth knowledge of canine anatomy, and so should only be done by a veterinarian or under the direct supervision of a veterinarian by someone who has been trained in this procedure.
Piglet’s experience
I wanted very much to try this new form of therapy with my dog, Piglet, about whose arthritis I’ve written in the past (see ”Joint Decisions,” March 2007). While Piglet has done remarkably well with a homemade diet, natural supplements, and prescription medications, she had slowed down several months earlier and was no longer taking long walks, cutting some as short as 20 minutes.It was difficult to find a veterinarian in my area who offers shock wave therapy for dogs. The nearest vet school uses it for horses, but has not yet tried it for dogs. Efron suggested I contact the companies who make the devices to see if they could help, and one company gave me the names of two vets within driving distance.
I took Piglet to Dr. Jeffrey Smith, current President of the California Veterinary Medical Association, of Middletown Animal Hospital in Middletown, California. Dr. Smith has used ESWT to treat horses, dogs, and even a goat, with great success.
“About 80 percent of animals show marked improvement post treatment, though it may take up to 90 days to see this,” Dr. Smith told me. “Ideally, treatment is repeated annually. Even in cases where no improvement is achieved, there are no negative side effects as one might experience with surgery or drug therapy."
Dr. Smith recommended two treatments for Piglet, one month apart. While he usually treats dogs under heavy sedation, we decided to use general anesthesia, due to my concern about Piglet’s noise phobias, as well as her age and breed. The treatment went well, with only minor increased soreness for a day or two afterwards, possibly due to the long drive.
Unfortunately, Piglet did not experience marked improvement, possibly because of the excessive amount of bony growth around her joints. I didn’t notice any changes following the first treatment, but two weeks after the second treatment, Piglet unexpectedly walked for twice as long as she had in many months. For half a year now, she has continued to take periodic long walks, up to two hours, every week or two, though most walks are closer to an hour.
Even without the marked improvement I had hoped for, I’m still glad that I tried it. The treatments were not hard on her, and I felt confident that they would do no harm. The improvement that she gained, while small, was meaningful and has allowed her to enjoy her walks more than before. At 16 years old, she’s still remarkably healthy other than her arthritis, including being mentally sharp, and her walks mean a lot to her and contribute to her quality of life. If I had it to do over again, I would make the same decision in a heartbeat.
One dog’s remarkable improvement
Dr. Smith told me about another dog he had treated a year earlier. Utah is a mixed breed (perhaps Pit Bull and German Shepherd Dog), weighs 45 lbs, and was 11 years old when she received shock wave therapy.Utah’s owner, Jane Rosett, MD, of Kelseyville, California, gave me the details. “Utah had problems with one elbow for many years, eventually reaching the point where she couldn't put weight on the leg at all,” says Rosett. Like Piglet, Utah was given two shock wave treatments, one month apart. "I didn’t see any improvement after the first treatment, and in fact I think she got a little worse. I was disturbed, as I thought I would see progress right away, but Dr. Smith explained that it can take some time for bone changes to take place,” Rosett continues.
Then it happened. “Two to three weeks after the second treatment, she suddenly began running around like a puppy again!” says Rosett. “The improvement was rapid and dramatic, and she’s been sound ever since, with only occasional mild limping."
Rosett offered a recent update on her 12-year-old dog, about a year and a half after the treatment. “Utah had been doing so well that I hadn't been giving her any medicine at all until a few weeks ago, when she began limping off and on. I'll probably be taking her to see Dr. Smith for another treatment soon.”
Mechanisms for generating shock waves
There are three types of ESWT devices, which generate high-energy, focused shock waves. They consist of electrohydraulic, electromagnetic and piezoelectric devices. All of these mechanisms convert electrical energy into a pressure wave within a fluid media (the body). No significant difference in effectiveness between these different methods of producing shock waves has yet been demonstrated. The FDA has approved electrohydraulic devices for treatment of multiple conditions in humans. Both Dr. Schenck and Dr. Smith use the VersaTron electrohydraulic device.A fourth type of device produces low- to medium-energy radial waves, also called ballistic or pressure waves. This type of treatment is most accurately called radial pressure wave therapy (RPWT), but is also sometimes referred to as radial shock wave therapy (RSWT), unfocused shock wave therapy, or grouped together with ESWT. RPWT utilizes a projectile mechanism to stimulate a pressure wave.
Focused shock waves and radial pressure waves differ mainly in terms of the energy type and penetration depth. Shock waves produce maximum energy at the focal point inside the tissue, while the maximum energy of pressure waves is delivered to the skin surface and dissipates from there. For this reason, radial pressure waves are most suitable for treating areas near the surface. Because pressure waves radiate outward from the point of origin, they affect a broader area than focused shock waves, which can be more effective for certain conditions, such as dissolving tendon calcifications.
More treatments with less time in between are needed when using RPWT. Less sedation is required due to the lower intensity of the pressure waves, which cause less pain than higher-intensity waves. Most studies in the US have been done using ESWT, which are the only devices approved by the FDA for treating humans. Both device types are widely used in Europe.
Soft-focused waves
Manufacturers have begun developing new delivery heads to provide a wider variety of treatment options for various musculoskeletal needs. Now, there are devices that allow use of either a focused or soft-focused therapy head, depending on the area being treated.Practitioners at the Toronto Equine Hospital in Toronto, Ontario, have used shock wave therapy on horses for the past eight years. Tami Packham, a technician there, became interested in its use in canine conditions after reading studies done by Iowa State’s Dr. Scott McClure. Packham approached the hospital’s Dr. Darryl Bonder, and with his help launched a pilot project where the machine and a technician are contracted to small animal veterinarians in the area. Acceptance by small animal veterinarians has been slow, with word-of-mouth among owners being the driving force behind most treatments.
The manufacturer says that the soft-focused waves are non-painful and can be applied without anesthesia or sedation, though this is questionable. “I have seen dogs treated with both focused and soft-focused waves, with and without sedation,” says Packham. “Even with soft-focus, the treatment can be painful, so I prefer that dogs be sedated and given pain medication before treatment.” In addition, some areas, such as the hips, can be difficult to treat without sedation due to the positioning required of the dog.
Packham describes the difference between the two types of treatment. “The focused head has a band width of 6mm, while the soft-focus head has a 25mm band width. The energy level is the same but more intense coming through the 6mm band as opposed to the 25mm band. I have tested both heads on myself and found them both painful.” Note that soft-focused waves are true shock waves, not radial pressure waves, which are less intense than any shock waves.
Search and rescue dog improves
Zeus, a German Shepherd dog who was trained and FEMA-tested for urban search and rescue, is owned by Rob and Shari Martin. “Zeus was x-rayed at age two, and found to have grade-4 hip dysplasia, as well as elbow problems,” says Rob Martin. “His ability to work declined, and within a year, he was in so much pain that we were considering euthanasia.”That’s when they met Packham. She explained about shock wave therapy to the Martins, who decided to try it for Zeus. After a single treatment, Zeus returned to about 80 percent of normal function. “Even though he could no longer do search and rescue, we were thrilled that he could enjoy a normal life as our pet,” says Martin.
Six months later, he began to decline again, and by the end of a year he was back to where he started, so the treatment was repeated.
“Zeus was retired at age three due to severe dysplasia in both hips and elbows,” says Packham. “Zeus has been treated for the last three years, one session each time. He continues to receive a treatment session about once a year.” Zeus is now 6 years old and has received a total of four treatments.
Martin describes Zeus’s response to treatment. “For the first three days after a session, he is like a puppy again, apparently due to the numbing effect of the treatment. During that time, we have to be careful that he doesn’t overdo it. Over the next three or four days, he seems to have a lot of pain, even worse than before the treatment. He then begins to improve again, and by about the 10th day following treatment, he is zipping around with about 70 to 80 percent of normal function.” Martin says that the short-term regression a few days after treatment was not as bad when soft-focused waves were used.
Zeus has received treatment with and without sedation, but Martin feels he does best when sedated, which allows higher-intensity waves to be used. “The effects seems to last longer when he is sedated,” says Martin. “It takes about eight months before he began to decline again, compared to six months following the lower-intensity treatment without sedation.”
ESWT for spondylosis
Hayley is a 12-year-old Golden Retriever who was in so much pain from spondylosis (fused vertebrae) that the family was considering euthanasia. She had difficulty getting up, and controlling her rear legs.“We noticed rather rapid deterioration in Hayley's movement last fall,” says Hayley’s owner, Christine Crooks, of Binbrook, Ontario. “She would take up to ten minutes to get out of her bed. When she walked through a door and turned, the back half of her body would not follow and she would fall. When she lay on the ground to rub her back and tried to kick her legs up in the air, only the front half would go up, while the bottom half just lay there. She had difficulty going up and down the stairs. And she looked just plain sad. She also had trouble lying in one place for long.”
Packham told the Crooks about shock wave therapy, and Hayley received a single treatment in November. She experienced a lot of pain after the procedure and had to take pain medication for two or three days.
“About a week after her procedure, I noticed that she was getting up effortlessly,” says Crooks. “Throughout the next week, we noticed constant improvements – she would walk out a door and turn, and her whole body would follow. She almost ran up and down the stairs. But the day that I started crying with emotion was the day that she lay on the ground and kicked all four legs up in the air.”
Crooks says this treatment has had a remarkable effect on Hayley’s life. “Her disposition improved greatly – we all talk about how our 12-year old dog is like a puppy again. Our veterinarian even said that we have to slow her down a bit to prevent her from injuring her spine. She likes to run in the snow and jump if we throw a snowball, so we have to remember that she still has a condition. To date, four months after the treatment, she continues to do remarkably well.”
Packham says, "The dogs go home with pain medication because they are usually very sore for three days post treatment. On average, we see improvement that lasts for six to eight months, and then they start to degenerate again." At that point, the treatment can be repeated.
Cost of treatment
The cost for ESWT can vary considerably, depending on which type of machine is used, how many sites are treated, whether your dog is anesthetized or just sedated, and what tests are needed before treatment. The lowest price I’ve heard of was $125 for treatment with RPWT without anesthesia (devices that generate radial pressure wave are less expensive and therefore the treatment may also be less expensive, though more treatments are usually required). Treatment with ESWT will commonly run around $200 to $300 per site, plus the costs for exam, tests, pain medication, and anesthesia or sedation.To give examples, Efron paid $425 per treatment for Taylor, with each treatment covering multiple sites. I paid $290 per treatment site (total $580 for both elbows) each visit. These prices do not include charges for sedation/anesthesia, pain medication, tests or exams.
Taylor, 8 months later
Taylor, the Lab who is owned by the people who originally asked me about ESWT, is still doing well, eight months after treatment. “Taylor is on no medications, but she gets a lot of supplements and a raw diet,” says Efron. “I think her improvement peaked about eight weeks after the second treatment, and she’s been great on walks ever since. We went to the beach last weekend. Taylor was so energetic and she was begging me to throw a ball. I threw one five feet and she trotted to retrieve and was happy as can be. Then my husband threw a leash and she ran a little. She was so happy and like a puppy again. I had tears in my eyes. Nothing makes me feel better than to see her like this.”How to find a practitioner
Because ESWT is still considered experimental, especially in dogs, it can be difficult to find a veterinarian who offers it. I recommend asking the device manufacturers to if they have sold any to vets in your area; contact information is listed under Resources below.You can also try contacting veterinary schools and large-animal vets in your area. Because shock wave therapy is used more commonly with horses, you might find a large-animal veterinarian who is willing to treat your dog, which can be done in cooperation with your own vet if needed.
I regret that I no longer have much time to respond to questions. See my Contact page for more information. My name is Mary Straus and you can email me at either or
